Liver Cirrhosis Support
Liver cirrhosis involves progressive scarring of hepatic tissue. Regenerative medicine explores supportive roles using MSCs to assist in inflammation modulation, immune regulation, and hepatic microenvironment optimization.
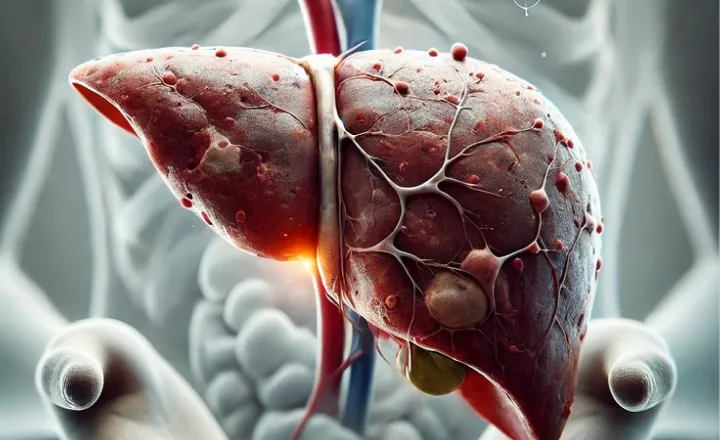
Introduction to Hepatic Support
Liver cirrhosis is a chronic condition characterized by progressive scarring (fibrosis) of liver tissue, often resulting from long-term liver injury such as hepatitis, alcohol-related liver disease, fatty liver disease, or autoimmune disorders. As healthy liver tissue is gradually replaced with scar tissue, liver function may decline over time.
Management typically involves hepatology supervision, medication, lifestyle modification, monitoring of liver function markers, and in advanced cases, transplant evaluation. Cirrhosis is a serious medical condition that requires continuous specialist care. Regenerative medicine approaches using mesenchymal stem cells (MSCs) are being clinically explored as supportive adjunct strategies within a comprehensive medical plan.
How MSCs May Provide Support
Mesenchymal stem cells (MSCs) are being clinically studied for their potential role in:
Hepatic tissue environment support
Systemic inflammation modulation
Cellular signaling balance
Immune system regulation
In cirrhosis settings, MSC therapy is explored as a supportive adjunct approach aimed at optimizing the liver microenvironment and assisting inflammatory regulation pathways.
It is important to note:
stem cell therapy does not reverse cirrhosis
It does not regenerate scarred liver tissue into normal tissue.
It does not replace transplant evaluation or hepatology care.
Individual responses vary depending on disease stage and overall health status.
Combination Therapy (If Applicable)
Depending on the individual case, supportive adjunct therapies may be evaluated to assist systemic inflammatory balance and metabolic regulation. Any complementary approach is considered within a comprehensive hepatology-guided plan.
Treatment Process
A typical regenerative pathway for Liver Cirrhosis includes:
1
2
3
4
5
6
7
All protocols are individualized and aligned with the patient’s treating liver specialist.
Safety & Eligibility
Eligibility depends on:
Stage of cirrhosis
Current liver function stability
Stage of cirrhosis Current liver function stability
Overall medical condition
Patients with advanced or unstable cirrhosis require careful screening. Regenerative therapy is considered only when medically appropriate and safe.
Stem cell therapy for liver cirrhosis is:
A supportive adjunct therapy
Not a replacement for medical management
Not an alternative to transplant when transplant is indicated
FAQs
Free Online Medical Consultation
Speak with a medical advisor and receive a personalized evaluation based on your medical reports. No obligation — professional guidance to help you understand available regenerative treatment options.
Book Free Consultation